Healthcare Use Case
The planning, budgeting, and forecasting system built for healthcare.
Workday Adaptive Planning gives healthcare organizations the planning, budgeting, forecasting, and modeling system powerful enough to plan for whatever comes next.
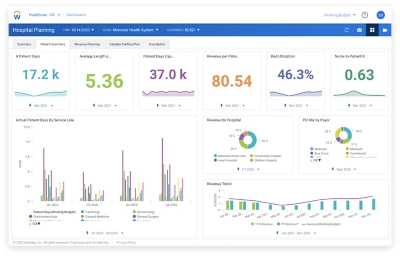
Key use cases.
Explore models built for healthcare.
-
Major volumes and units of service forecasting—Acute care providers, physician practices, and skilled nursing facilities can plan admissions, patient days, visits, cases, RVUs, and occupancy rates.
-
Net revenue modeling—Plan gross patient revenue, contractual allowances, charity care, reimbursement across service lines, patient types, and payors.
-
Cost management—Budget fixed and variable labor, COLA adjustments, supplies, bad debt, and maintenance expenses.
-
Staff and workforce planning—Plan FTEs, retention, turnover, as well as compensation, benefits, taxes, and other costs for salaried and hourly workers. Integrate HR and payroll systems to pull in employee data and utilize multiple fringe rate assumptions.
-
Labor productivity—Model shifts, productive, and unproductive time as well as units of service to drive improvements in labor productivity.
-
Supply and demand planning—Match medical and surgical supply requirements based on patient volumes with purchasing and inventory management. Align procurement strategy and cost with profitability of procedures/services and assess contingency product options.
-
Service line profitability—Segment volumes, revenue, and direct costs by line of service, and allocate head count and overhead to track profitability.
Ready to talk?
Get in touch with us.